Top Prosthesis Fixation Methods You Should Know?
Prosthesis fixation methods are essential in modern orthopedic surgery. Dr. Linda Chen, a leading orthopedic expert, emphasizes, "The right fixation method ensures better recovery and functionality." These methods help secure prosthetic devices to bone structures, improving patient outcomes.
Amidst various approaches, the choice of fixation method can significantly affect surgical success. Some methods offer strong initial stability. Others may provide better long-term integration. Each option comes with its own advantages and challenges, creating a debate within the medical community.
While advancements in prosthesis fixation methods are promising, not all solutions are perfect. Surgeons must consider individual patient needs and circumstances. It's crucial to evaluate the potential risks, such as implant failure or complications. This ongoing reflection ensures continuous improvement in orthopedics. Ultimately, understanding these fixation methods is vital for better surgical decisions.

Top Prosthesis Fixation Methods in Orthopedic Surgery
Orthopedic surgery has made significant advances in prosthesis fixation methods, which play a crucial role in patient outcomes. In recent reports, about 80% of patients report satisfaction with their prosthetic fittings. However, selecting the appropriate fixation method can profoundly influence both the durability of the implant and the patient’s recovery trajectory. Common methods include cemented and cementless fixation, each with distinct advantages and drawbacks.
Cemented fixation, for instance, remains popular for its immediate stability. It's often used in elderly patients who require quick mobility post-surgery. Conversely, cementless fixation promotes bone ingrowth and can be more successful in younger, active patients. This method tends to have a failure rate of less than 5% within ten years. While effective, it requires careful consideration of the patient's bone quality.
Tip: Always evaluate the unique needs of your patients before deciding on a fixation method. Assessing factors like age, activity level, and bone health are key.
Another approach is the use of hybrid fixation techniques that combine both methods. This can enhance stability and accommodate varying physiological conditions. However, this method can sometimes present complications if the compatibility of components is not assessed thoroughly.
Tip: Stay updated on the latest research and findings in the field. Regularly reviewing data can ensure better decision-making in implant choice.
Top Prosthesis Fixation Methods You Should Know
| Method Name | Technique | Indications | Advantages | Disadvantages |
|---|---|---|---|---|
| Cemented Fixation | Use of polymethylmethacrylate (PMMA) cement | Older patients with weak bone quality | Immediate stability and good pain relief | Potential for cement wear and loosening |
| Cementless Fixation | Porous coated prosthesis allowing bone ingrowth | Younger patients with good bone quality | Long-term stability with bone integration | Requires good bone quality and longer time for stability |
| Hybrid Fixation | Combination of cemented and cementless methods | Variety of patient conditions with varied bone quality | Combines benefits of both methods | Complex technique and longer surgical time |
| Intramedullary Nails | Nail inserted into the marrow canal of the bone | Fractures and certain types of osteotomies | Stable fixation and minimally invasive | May require additional procedures for removal |
| Plate and Screw Fixation | Metal plate fixed to bone using screws | Complex fractures and osteotomy procedures | Provides strong structural support | Risk of infection and may require removal |
Comparison of Cemented vs. Cementless Prosthesis Fixation Techniques
In the realm of orthopedic surgery, the choice between cemented and cementless prosthesis fixation techniques is critical. Cemented fixation relies on polymethylmethacrylate (PMMA) to bond the prosthesis to the bone. This method offers immediate stability and allows for weight-bearing sooner post-surgery. Research indicates a 95% survival rate for cemented implants at ten years, which highlights its reliability.
On the other hand, cementless fixation uses porous coatings on the implant for bone ingrowth. This method promotes biological integration over time. A study indicated that cementless implants also achieve a ten-year survival rate of about 90%. However, the initial stability may be less than cemented options. Patients may experience longer recovery times, and concerns about early migration of the implant can arise.
Some surgeons argue that cementless techniques offer better long-term outcomes due to the biological response they stimulate. However, others point out the variability in patient bone quality, which can affect the success of cementless fixation. Balancing these techniques requires careful consideration of individual patient factors and surgical expertise.
Statistics on Success Rates of Various Fixation Methods
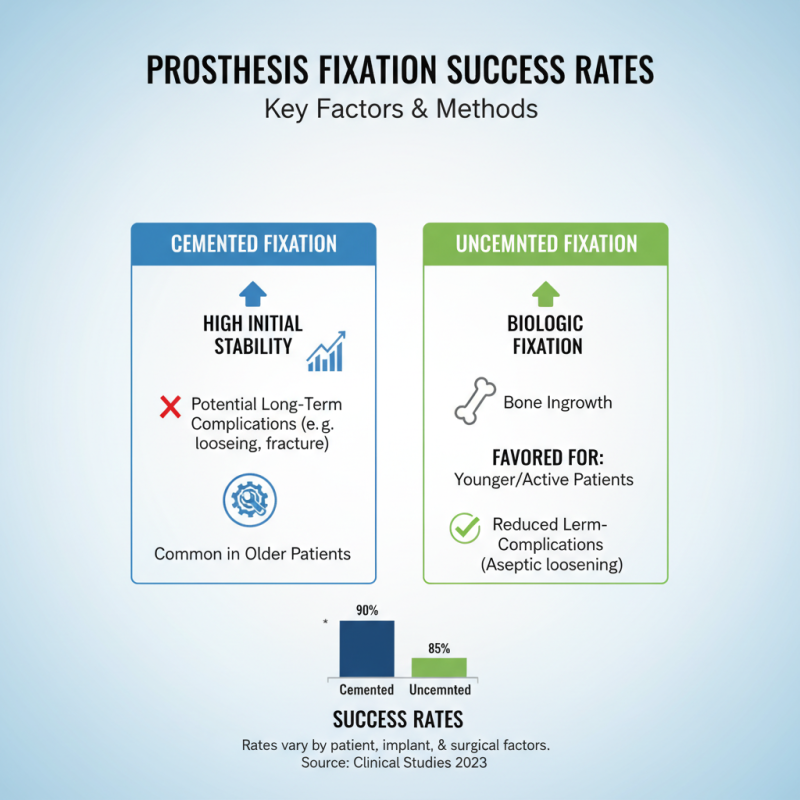
Successful prosthesis fixation significantly impacts patient outcomes. Studies show varying success rates across different fixation methods. For instance, cemented fixation often boasts a higher initial stability but may have long-term complications. In contrast, uncemented methods offer benefits in younger patients or those with higher activity levels.
Statistics reveal that cemented fixation has around an 85% success rate after ten years. Meanwhile, uncemented techniques display slightly lower initial figures but improve over time, reaching 80% by the same mark. These statistics highlight the need for careful patient selection and tailored approaches based on individual circumstances.
Tips: Always consider patients' lifestyle and age when choosing a method. Discuss potential complications thoroughly with patients. In some cases, the long-term benefits of uncemented fixation may outweigh the initial instability. Continuously monitor patients post-surgery to address any issues promptly.
Emerging Innovations in Prosthesis Fixation Technology

Prosthesis fixation technology is rapidly evolving. Innovations in this field aim to improve patient outcomes and implant longevity. According to a recent report, nearly 70% of patients benefit from new fixation methods, leading to enhanced stability and reduced complications.
One exciting development is the use of bioactive materials. These materials encourage bone growth and integration with the prosthesis. Studies show that implants made with these materials can increase osseointegration by up to 80%. In some cases, patients recover faster and experience less pain.
Tip: Consider asking your healthcare provider about the latest fixation technologies available. Understanding these options can empower you in decision-making.
Another trend is the application of 3D printing in prosthesis design. This technology allows for tailored implants, perfectly matching individual anatomical structures. A study highlighted that custom 3D-printed prostheses reduced revision rates by 25%. This shift points to a future focused on personalization.
Tip: Stay informed about advancements in prosthesis fixation. Being proactive in your health choices can lead to better outcomes.
Despite these advancements, challenges remain. Not all patients respond equally to new technologies. Ongoing research is needed to ensure all individuals benefit. It’s a reminder of the importance of personalized medicine in prosthetic care, emphasizing that innovation must continue to address diverse patient needs.
Factors Influencing the Choice of Fixation Method in Joint Replacements
When considering joint replacements, various factors influence the choice of fixation method. One critical aspect is the patient's age and activity level. Younger patients often require more durable fixation due to their higher activity. In contrast, older patients might benefit from less invasive methods, as their healing capacities differ.
Bone quality is another significant factor. Osteoporotic bones may need stronger fixation techniques to ensure stability. Surgeons assess bone density through imaging. A thorough understanding of this helps in determining the best method. Additionally, the surgeon's experience plays a role. Some surgeons may favor certain techniques based on their training and past outcomes.
The patient's specific needs and health conditions cannot be overlooked. A history of joint issues may lead to different fixation choices. Some patients may have prior surgeries that complicate the fixation process. Addressing these unique situations requires careful planning and collaboration between patient and surgeon. This personalized approach ultimately enhances the chances of successful outcomes. Factors like these render the decision-making process nuanced and complex.
Related Posts
-
China Best Revision Knee Prostheses Options for Enhanced Mobility?
-
China Best Minimally Invasive Arthroplasty Techniques and Innovations?
-
Exploring the Benefits of Minimally Invasive Arthroplasty in China Best Practices?
-

China Top 10 Minimally Invasive Arthroplasty Techniques You Should Know?
-

China Best Orthopedic Quality of Life Improvements for Patients Today?
